Overactive Bladder (OAB)
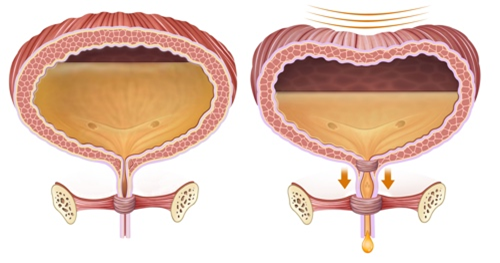
Overactive bladder is a condition which has a group of urinary symptoms which causes urgency, urge incontinence, frequency and need to wake up from sleep to pass urine. In most cases no cause is identified, however it may be secondary to bladder obstruction due to BPH or a neurological condition.
You will have a thorough history and examination to determine the issues pertinent to your condition. A bladder diary is important to gain information about your bladder for a 24 hour period prior to review, also a flow rate and bladder scan. You may require a flexible cystoscopy depending on your symptoms and further investigation with urodynamics.
Treatment can include conservative options if not trialled, or various medications. After further investigation for urodynamics , you may be a candidate for minimally invasive surgical options. These include intravesical botox or sacral neuromodulation
Stress Urinary Incontinence
Urinary incontinence is a common problem in both men and women. Stress incontinence is leakage of urine which occurs during moments of physical activity that increases abdominal pressure such as sneezing, laughing or exercise.
You will be assessed by your surgeon as to whether further investigation is required. There are conservative and surgical options which are available to help you.
Urinary Tract Infections
A Urinary tract infection (UTI) is a bacterial infection of the bladder (cystitis). Cystitis can spread to involve other organs in the urinary tract, including the kidneys (pyelonephritits), prostate (prostatitis) and testes (orchitis).
UTIs’s are relatively common in women. WHen they occur three of more times a year, they are considered recurrent UTIs. Recurrent UTIs may require further investigation or treatment.
UTIs in men are uncommon and after often a sign of a problem with the urinary tract and may warrant further investigation or treatment.
You will be assessed with a thorough history and examination and determine if you require more investigation.
More information on Recurrent Urinary tract infections
Scrotal masses and swelling
Swelling and masses in the scrotum are common and can be caused by a number of conditions including hydrocele, epididymal cyst, varicocele, inguinal hernia, infections and testicular cancer.
Most scrotal masses are not serious or dangerous, it is important to see a GP or urologist to investigate a new scrotal swelling. If you require surgeries, this will be a hydrocele and epididymal cyst repair and varicocele repair.
More information about scrotal lumps